Sedera Montgomery stands at the front, ready to start the day’s discussion: how to help stop a fatal opioid overdose with naloxone, a medication most commonly known as Narcan — its brand name.
“These are some of the signs and symptoms that you would see if a person was suffering from an overdose,” Montgomery says to the room of second and third-year medical students. “Their skin could be clammy, there could be loss of color, their lips and fingertips could be blue — they could be blue all over, depending on how long they have been without oxygen.”
Montgomery says if you suspect someone is having an overdose, the first thing to do is call for help. Then, she says, keep an eye out for signs that the overdose could turn fatal.
“Two cardinal signs are pinpoint pupils and this thing that I call a ‘death rattle,’ this deep, gurgling-type snore,” Montgomery says. “When that happens, you should be ready to act.”
Though you wouldn’t expect it, Montgomery later admits she was a little nervous during her presentation. She isn’t a professor at the school or a physician in a white lab coat. She’s a trainer with a nursing background who works for the Louisiana Department of Health’s Metropolitan Human Services District.
But Montgomery’s experience with treating overdoses makes her the perfect person to teach this subject. As the number of opioid overdoses in the Gulf South has risen over the past two decades, she’s witnessed the worst of the worst. This intimate knowledge of death wrought by the opioid crisis is apparent in the way she carries herself: upright and commanding, with the no-nonsense vibe of a high school principal.
Louisiana’s overdose death rate is nearly double the national average, and 95% of those deaths were caused by fentanyl — a synthetic opioid often mixed with other drugs to make the mixture stronger. Fentanyl is about 50 times more potent than heroin, making it easy to unintentionally take a deadly amount.
It’s an epidemic that does not discriminate, devastating entire communities regardless of age, sex, race, or socioeconomic status.
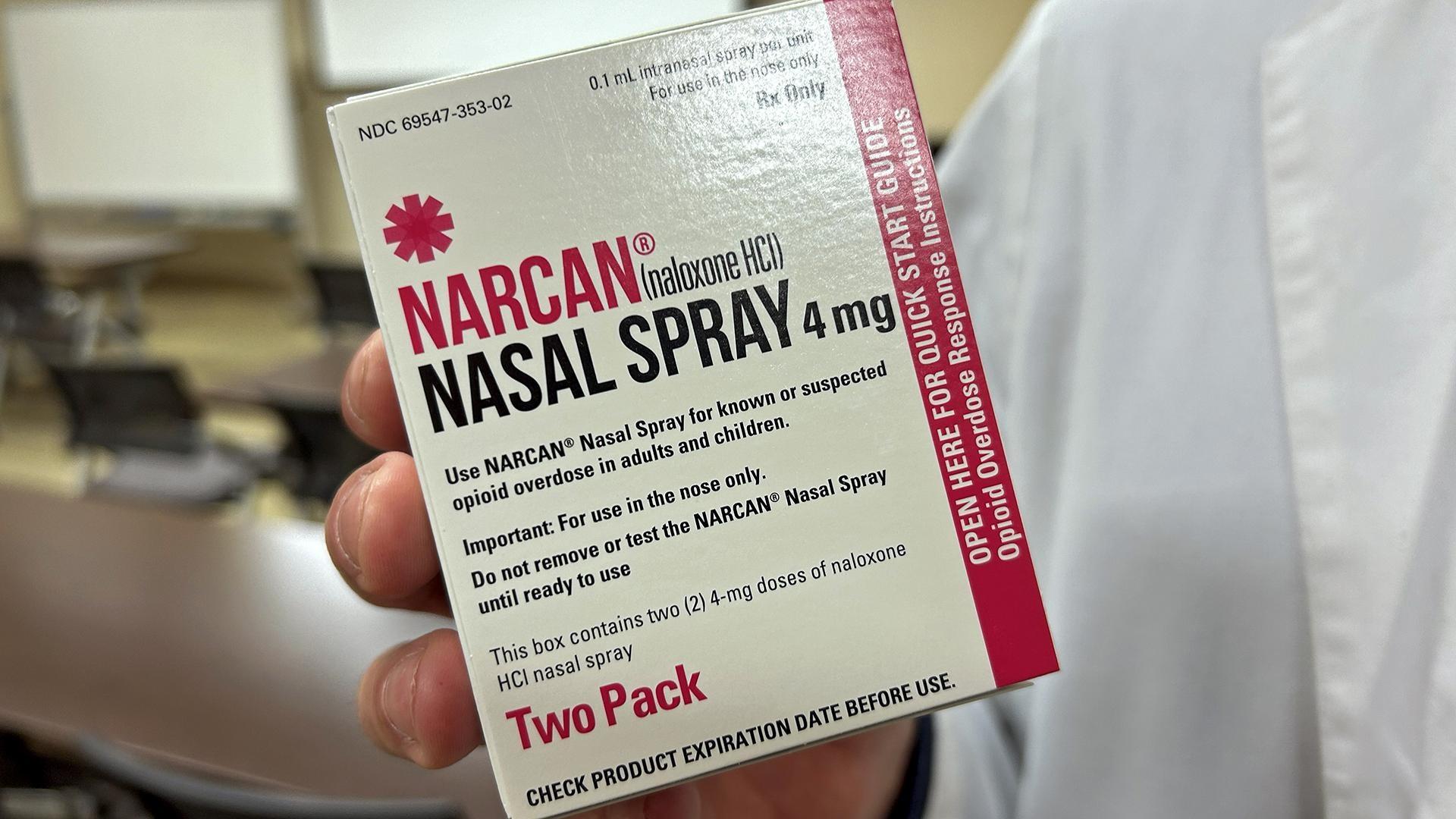
Montgomery continues the training by opening a box and pulling out a small device with a nozzle. It looks like a nasal spray bottle for allergies, but it’s actually a dose of naloxone. Spraying the drug directly into the nostril allows it to enter the bloodstream and take effect within seconds. This ability to quickly reverse a potentially fatal opioid overdose has led to some calling it a “miracle drug.”
“This is how you hold it,” Montgomery says, gripping the device. “Your thumb is on the plunger and ready to go.”
She then shows the students how to deliver a dose.
“Make sure it’s in the nostril.”
A student raises their hand and asks how you’d know if the device was in far enough. Your fingertips will touch the tip of that person’s nose, Montgomery replies.
“And once you get it there, you press,” she says, pressing the plunger and sending a small puff of mist rising into the air.
Each Narcan device contains a single dose of naloxone. Montgomery says it can sometimes take multiple doses to revive someone, though one can often do the trick.